The inspiring story of Willem Kolff, inventor of dialysis!
This video explains why we urgently need to transform the way we prevent and treat kidney disease.
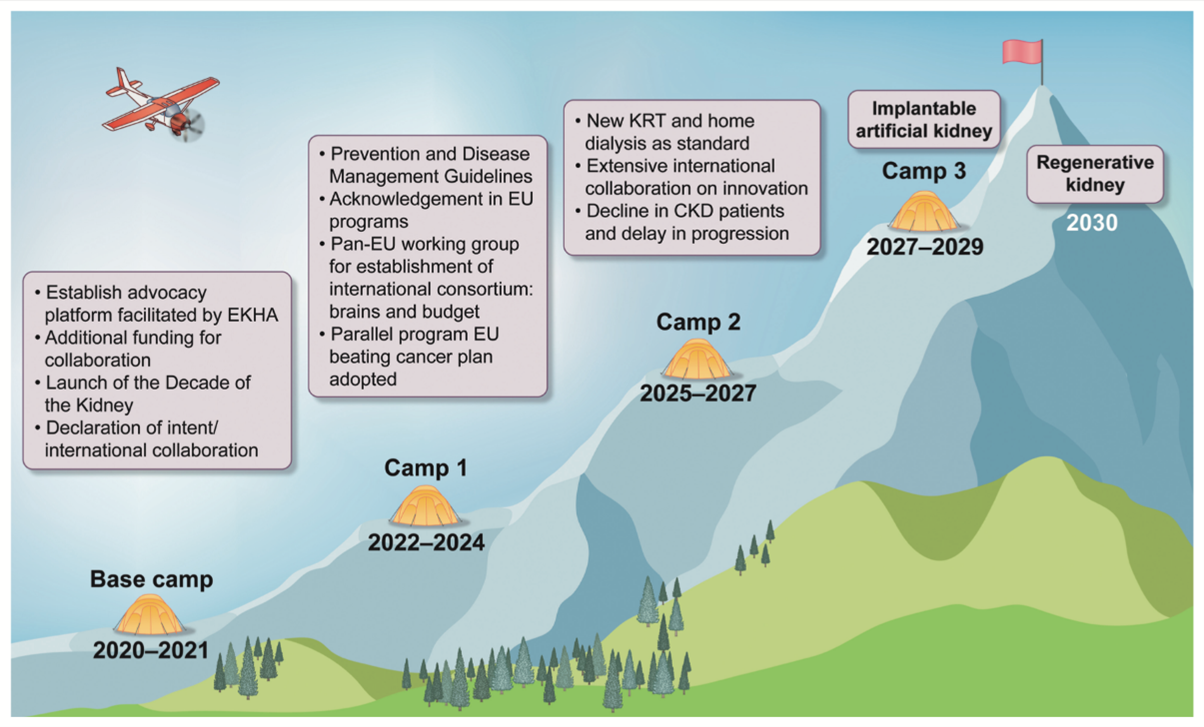
Health is an essential indicator of any country’s prosperity. But in our aging societies, healthcare systems need a paradigm shift to cope with increasing demand and spiraling costs. In Europe, nearly 100 million people suffer from chronic kidney disease. Current predictions are alarming. Today, CKD is one of the most expensive diseases for healthcare systems to treat, and dialysis has a substantial ecological impact.
To remain sustainable, kidney patient care must shift from reactive hospital treatment to proactive prevention and home-based therapies.
This is the story of next-generation artificial organs, which are already well advanced. With relatively small investment, they can transform the lives of millions of kidney patients worldwide.
To understand the importance of this journey, we travel to the Dutch province of Overijssel, to the city of Kampen — the birthplace of artificial organs.
This year, we celebrate the pioneers who made the first breakthroughs in kidney replacement therapy.
It began 80 years ago in the Netherlands, in the city of Kampen. During the Second World War, a young Dutch doctor refused to work with the Nazis. He also refused to accept the medical view of that time that nothing could be done for patients with kidney failure.
As a result of his courage and dedication, Dr. Willem Kolff’s inventions keep millions of people alive today. His way of working still inspires the Dutch Kidney Foundation to keep pushing for new developments.
Before we begin, let us understand kidney failure through the story of a dialysis patient named Philip.
Philip undergoes dialysis three times a week because his kidneys are severely damaged. Healthy kidneys remove waste products and excess water from our blood and excrete them in the urine. They also regulate blood pressure, blood sugar, and the body’s acidity.
When kidneys fail, as in chronic kidney disease, waste removal decreases dramatically. Waste accumulates in the blood, damages organs, and causes severe illness. When kidney function falls below 15 percent, survival requires either transplantation or dialysis.
Transplantation is the best option, but there is a shortage of donor organs, and not every patient qualifies. Therefore, dialysis remains the main therapy.
Let us go to the place where dialysis was invented by Dr. Willem Kolff, later known as the father of artificial organs.
We are in Kampen, a city along the River IJssel in the Netherlands. This is the hospital where it all happened. Our host, Herman Broers, wrote a biography about Dr. Kolff.
In 1942–1943, Kolff built the rotating drum artificial kidney. The replica still exists. The original version used aluminum from a downed aircraft. Later versions used different materials due to shortages during the war.
The patient was connected via rubber tubing. Blood was pumped through cellophane tubing and rotated in a dialysis bath. Waste products moved across the membrane into the dialysis fluid.
The first successful dialysis session lasted 13 hours. Approximately 80 grams of urea were removed. Watching a patient regain consciousness after such treatment was extraordinary.
Kolff’s motivation came from witnessing the death of a 22-year-old patient from renal failure. As a young physician, he had to tell the patient’s mother that nothing could be done. That moment changed him.
He calculated that if he could remove approximately 20 grams of urea per day — the amount produced — a patient might survive. Though the young man died, Kolff began working toward a solution.
When the Nazis invaded the Netherlands in 1940, Kolff refused to work under Nazi authority and moved to Kampen. It was a small town with 19,000 inhabitants and only one hospital doctor. Kolff became the second.
The town’s isolation allowed him to continue his work.
Using cellophane tubing — originally sausage casing — he created a semi-permeable membrane. Small molecules such as urea diffused into dialysis fluid, while electrolytes could be balanced.
He determined that about 10 meters of tubing were needed and that blood had to remain in constant motion. He also had to prevent clotting. The result was a machine with sufficient surface area to remove waste effectively.
Kolff recruited a local team based on skills rather than diplomas. Sister Maria Terwiel, the head nurse, assisted him. Minneka from Groningen performed laboratory work. Andrew Scherbrant, a carpenter, helped build the device. Others joined from the local community and even from the resistance.
In March 1943, Janny Schroder became one of the first patients treated. On April 4, 1943, she regained consciousness from a uremic coma — the first documented recovery by hemodialysis.
Although she later died due to limitations in vascular access, the principle had been proven: dialysis worked.
The main limitation was vascular access. Kolff used glass cannulas and had to sacrifice blood vessels for each treatment. Chronic dialysis was not yet possible.
In 1960, Wayne Quinton and Belding Scribner in Seattle solved the vascular access problem. Together with Kolff’s machine, this breakthrough enabled chronic dialysis and has saved millions of lives.
Kolff never patented his invention. Instead, he built additional machines and sent them to Poland, England, Canada, and the United States.
In 1945, shortly after liberation, he treated a woman who had been a Nazi sympathizer. Despite political tensions, he believed every patient deserved treatment.
After successfully publishing his work in 1946, Kolff toured the United States in 1947 and 1948. He eventually moved to the Cleveland Clinic in 1950 to continue his research.
Later, he led the development of the first total artificial heart in Utah and became the first president of the American Society for Artificial Internal Organs (ASAIO) in 1955.
Kolff believed innovation requires courage, risk, and persistence. He often said inventions rarely happen while sitting at a desk — they come at four o’clock in the morning, or while cycling through the meadows.
His story reminds us that bold thinking, collaboration, and investment are essential for medical breakthroughs.
Today, as chronic kidney disease continues to rise worldwide, we need the same courage to rethink prevention, innovation, and patient-centered care.