Urine biomarkers could transform how we detect and manage chronic kidney disease
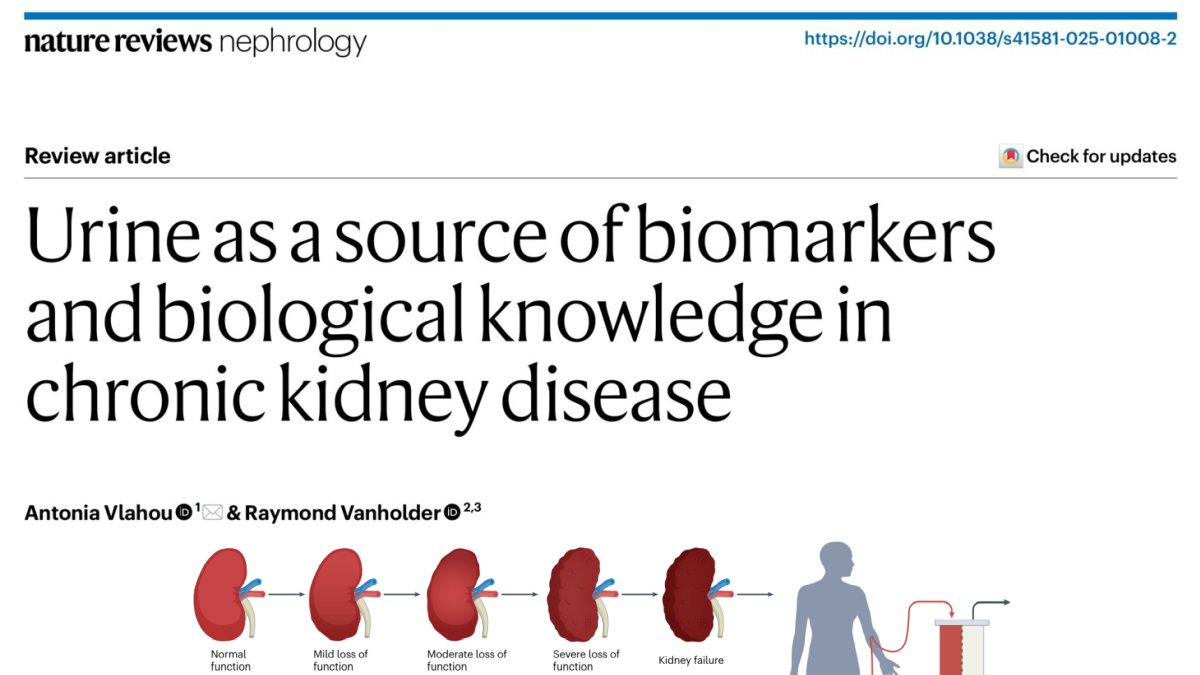
Chronic kidney disease affects hundreds of millions of people worldwide and often progresses silently until substantial kidney damage has already occurred. Current diagnostic tools such as albuminuria and estimates of glomerular filtration rate remain essential in clinical care, but they usually identify disease after injury has already developed and provide limited insight into the biological causes of kidney damage.
A recent review co-authored by the EKHA Past President Raymond Vanholder explores how urine analysis could change this situation by providing a much deeper view of kidney biology. The article highlights the growing body of research showing that urine contains a wide range of molecules that reflect what is happening inside kidney tissue. These molecules include DNA fragments, RNA molecules, proteins, peptides, and metabolic products released by kidney cells.
Because urine can be collected easily and non invasively, researchers increasingly view it as a potential “liquid biopsy” of the kidney. By analysing its molecular components using modern techniques such as proteomics, metabolomics, and genomic analysis, scientists can detect biological signals linked to inflammation, fibrosis, tissue injury, and cellular stress within the kidney.
Among the most promising candidates are protein based biomarkers that reflect processes such as tubular injury, immune activation, and tissue repair. Examples include markers such as uromodulin, kidney injury molecule 1, neutrophil gelatinase associated lipocalin, and chemokine ligand proteins. These markers may help identify disease earlier, estimate the risk of progression, and potentially guide treatment decisions.
Researchers are also developing multi marker panels that combine information from dozens or even hundreds of peptides. These panels aim to improve diagnostic accuracy by capturing several biological processes simultaneously. Some studies suggest that these molecular signatures may predict chronic kidney disease progression before traditional clinical markers change.
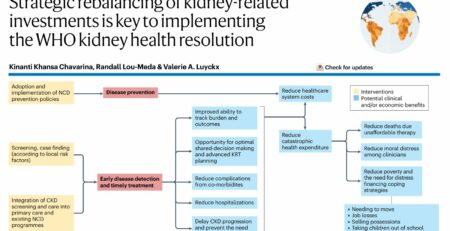
However, translating these discoveries into routine clinical practice remains challenging. Many biomarkers still require validation in large patient cohorts, and health systems must demonstrate that implementing these tests improves patient outcomes and is economically sustainable.
Despite these challenges, urine based biomarkers represent one of the most promising areas of kidney research today. As validation studies continue and analytical technologies advance, these approaches could support earlier diagnosis, better risk prediction, and more personalised treatment strategies for people living with chronic kidney disease.